My Blog
Anti-Aging Skincare: Ingredients and Techniques for Youthful Skin
- posted: Apr. 16, 2024
As we age, our skin undergoes changes such as reduced collagen production, loss of elasticity, and increased susceptibility to damage from environmental factors. While aging is a natural process, incorporating Read More
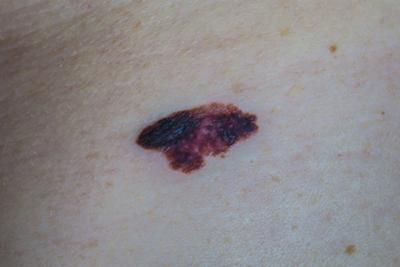
Mole Check: Importance of Regular Skin Exams for Early Detection
- posted: Apr. 03, 2024
Moles are common skin growths that can appear anywhere on the body. While most moles are harmless, changes in size, shape, color, or texture can sometimes indicate skin cancer or Read More
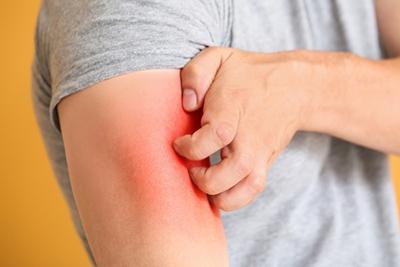
Are You Dealing with a Rash?
- posted: Mar. 08, 2024
Rashes can be itchy, uncomfortable, and ugly. They can develop suddenly or gradually over time. If you have a rash that doesn’t go away in a few days, you need Read More
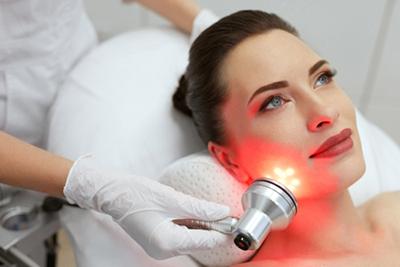
Introduction to Medical Skin Rejuvenation: A Comprehensive Guide
- posted: Mar. 06, 2024
If your skin is beginning to look dry and dull, you can do something about it. If you are embarrassed by acne or acne scarring, you can do something about Read More
What You Need To Know About Cosmetic Dermatology
- posted: Mar. 01, 2024
Cosmetic dermatology is focused on you looking your best. No matter what the aesthetic concern is, there is a procedure to help minimize the problem, so you can look great. Read More
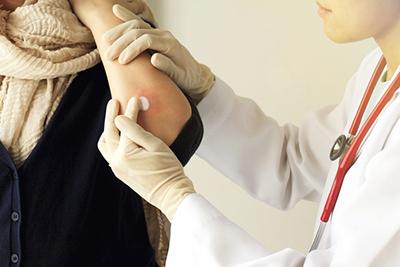
Skin Rash Treatment
- posted: Feb. 07, 2024
Seek Medical Help If You have a Skin Rash Dermatologists see patients with skin rashes. Please read on to discover the importance of visiting a dermatologist for your skin rash and Read More
Cosmetic Dermatology: Exploring Non-Surgical Aesthetic Procedures
- posted: Feb. 01, 2024
Cosmetic dermatology focuses on enhancing the appearance of the skin, offering treatments aimed at refining, rejuvenating, and correcting various skin concerns. Cosmetic dermatology doesn't revolve around vanity. It boosts confidence Read More
Eczema and Psoriasis: Understanding and Managing Chronic Skin Conditions
- posted: Jan. 11, 2024
Eczema and psoriasis are two troublesome, uncomfortable skin conditions your dermatologist can treat. Let’s look at the differences and similarities between these two conditions and how they are treated and Read More
Common Skin Conditions
- posted: Jan. 01, 2024
A dermatologist is a specialized medical professional focused on skin health. They're like skin detectives, trained extensively to diagnose, treat, and manage various skin, hair, and nail conditions. From acne Read More
Best Ways To Protect Your Skin
- posted: Dec. 07, 2023
Your skin is constantly exposed to different elements and it’s easy to deal with irritation or skin damage. Your skin is also susceptible to issues like skin cancer and it’s Read More
Managing Chronic Skin Conditions
- posted: Dec. 01, 2023
Chronic skin conditions can be embarrassing and uncomfortable. You may be able to manage a minor chronic skin condition on your own. For other chronic skin conditions, you can benefit Read More
FAQs About Melanoma
- posted: Nov. 07, 2023
Melanoma is a type of skin cancer. Skin cancer is the most common type of cancer, and it can be prevented and easily treated. It’s important that you understand melanoma Read More
Rosacea: Understanding Triggers and Effective Treatment Approaches
- posted: Nov. 01, 2023
Rosacea is a chronic skin condition causing redness, visible blood vessels, and sometimes bumps on your face. Its exact cause isn't clear, but triggers like sunlight, stress, spicy food, and Read More
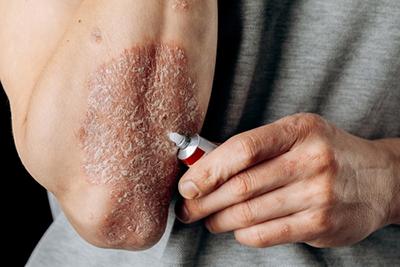
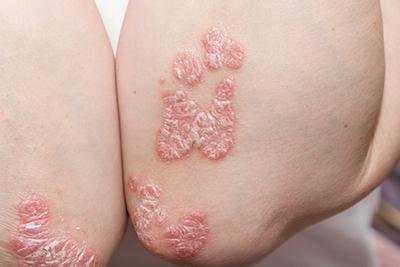
Suffering From Psoriasis?
- posted: Oct. 06, 2023
Psoriasis is a common skin condition affecting millions of people. It occurs when your skin cells multiply too rapidly, leading to thick, red, and often itchy patches called plaques. These Read More
What Can a Chemical Peel Do for Your Skin?
- posted: Oct. 01, 2023
A chemical peel is a cosmetic procedure in which a dermatologist applies a chemical solution to the skin to remove damaged outer layers, revealing smoother, more youthful-looking skin. Chemical peels Read More
Acne Treatment Options
- posted: Sep. 12, 2023
Acne is a common problem that people all over deal with. Dermatologists see acne problems every day and understand that it can be difficult to deal with. When you’re dealing Read More
This website includes materials that are protected by copyright, or other proprietary rights. Transmission or reproduction of protected items beyond that allowed by fair use, as defined in the copyright laws, requires the written permission of the copyright owners.
Our Location
Find us on the map
Seraly Dermatology
222 East McMurry Road
McMurray, PA 15317, US